MeritCare Health System’s Respiratory Therapy department (Fargo, ND) provides heartwarming care through management structure, therapist-driven protocols, and special programming.
By Liz Finch
Sitting on the prairie-rich eastern edge of North Dakota, the city of Fargo does not exactly conjure up pictures of cutting-edge respiratory care. According to the therapists on staff at the vicinity’s largest medical provider, however, this 175,000-person metro community is the home base of one of the largest physician group practices in the country. More impressive are the changes continuously under way within the respiratory care department at this medical hub.
“We are going through a positive growth experience here and are quite proud of what we do in our department,” says Jay Taylor, RRT, a critical care and lead respiratory therapist who joined the area’s MeritCare Health System almost 20 years ago.
According to Taylor, MeritCare is a place that stays on the leading edge of providing respiratory care to its patients. Recent growth experience for the department has included expanding its therapist-driven protocols (TDPs), and implementing a method of management that cultivates staff input and opinions, and the process of deciding on an entirely new fleet of ventilators also has begun.
“The therapists interact with the physicians, the nursing staff, and the patients. Through the TDPs, we have the ability to start treatments when needed and to change orders when necessary. We frequently add new things to the protocols; that means we get to utilize our skills as respiratory therapists. And everybody has a good sense of humor here,” Taylor says.
Humor certainly comes in handy in a place where the temperature stays below 50° 7 months out of the year, and dips to an average of 6° in winter. A 250-mile expanse of these frosty plains is served by the MeritCare Health System, which has 11 locations in Fargo/Moorhead/West Fargo, 14 regional locations in Minnesota, and 11 regional locations in North Dakota. Roughly 1.3 million patients visit these locations annually, and are treated by a staff that includes 352 doctors and 86 mid-level practitioners, including physician assistants and nurse practitioners.
In Fargo, where Taylor is part of the team of RTs, the respiratory care department plays a crucial role in two locations: the MeritCare Medical Center and the MeritCare Children’s Hospital. The Medical Center has a total of 583 licensed beds at two locations in Fargo, which includes 96 beds at Children’s Hospital.
The Respiratory Therapy Department, which initially opened in 1968, has 78 registered RTs serving in Adult Critical Care, Children’s Hospital, the Pulmonary Function Department, the Pulmonary Rehabilitation Department, and the Sleep Center.
MeritCare’s Respiratory Therapy Department and North Dakota State University jointly sponsor a respiratory care program leading to a bachelor of science degree, and an advanced-level respiratory therapist certificate. The faculty responsible for the curriculum for the school also coordinates and provides continuing education for staff therapists who serve as clinical preceptors for students. Approximately two thirds of the RTs hold a bachelor’s degree and the other one third have either an associates degree or a certificate of completion from an accredited respiratory therapy program.
The sheer range of departments that utilize respiratory services provide many challenging patient scenarios, according to Taylor. To keep things running smoothly, daily and shift assignments are made by a lead therapist utilizing a computer system. The workload is broken down into units and therapists are assigned various areas, depending on their expertise. Assignments are delivered at the start of each shift, which can be 8 hours or 12 hours long.
“Having 12-hour shifts in the level III neonatal intensive care unit (ICU) allowed for travel and other pastimes while maintaining a full-time job,” says Children’s Hospital coordinator Vickie Haberman, RRT. “ A few years later, working in education, and now in management, keeps me facing new challenges. Opportunity for mobility within the department is a major reason I am still working at MeritCare.”
Management Structure
Another appealing factor for the staff is the recently implemented Partnership Council approach to provide leadership and direction within the department. Staff representatives are elected annually and serve on the council with managers and coordinators to review department performance and provide direction for the future.
“I think the Partnership Council has improved our morale,” Haberman says. “People talk more, share more, and are involved with more in the department.”
They remain involved through the establishment of work teams, such as the equipment work team. That group recently reorganized the equipment room and streamlined the method by which items are brought to different floors. Another group, the recognition work team, focuses on acknowledging birthdays, anniversaries, and events like Respiratory Care Week in October.
“We put together a budget from the department itself for things like feeding the staff, providing door prizes, and putting up a couple of bulletin boards in the department,” Taylor says. “In this way, the department is taking the morale [problem] and addressing it as opposed to ignoring it. I don’t know a department in the world without a morale problem, it’s just the degree of the problem that varies.
“At MeritCare, the staff is taking an active part in fixing what’s wrong by making sure people are noticed,” Taylor adds. “Take our ‘Superstar Card,’ for instance, which staff members can fill out to recognize those who have gone above and beyond in their work. That costs nothing, but it is a way for the staff to pay attention to each other and respect one another.”
“Most of us spend more time here than we spend with our families, so we have to run the department a bit like families should run,” Haberman says. “This recognition program is a step in that direction.”
Therapist-driven Protocols
MeritCare took another step toward streamlining its respiratory care department in November 1987, when it implemented TDPs in the adult areas of the facility. The protocols are in use for about every area from mechanical ventilation to oxygen therapy to bronchodilator therapy. New ventilator TDPs include the use of the Ventilation Liberation Protocol (VLP), and Children’s Hospital also recently implemented a system called Respiratory Care Assess & Treat (RCAT).
“We are just getting into protocols for pediatrics this year, though we have been doing that all along by communicating with the physicians in this department,” Haberman says. “But this gives protocols to us on paper, and that means fewer phone calls, which is advantageous for the physicians.”
“We are at the place we are at with protocols because we started so early,” says Tamara McCabe Halvorson, RRT, respiratory department manager. “We use them as the norm [enabling] a therapist to be able to approach physicians about changes we want to make.”
A mechanical ventilation protocol work group and a TDP work group review the protocols on a monthly basis and make appropriate changes. Above all, the aim is to do the best thing for the patient, even if that means changing the treatment plan midstream.
“A couple of years ago I got frustrated with the changes that were always being made to the protocols, and I told Tamara I didn’t get it,” Taylor says. “She told me that 99% of protocols is using your head and doing what’s right. If you do what you’re trained to do, you’ll do the right thing.”
Choosing New Equipment
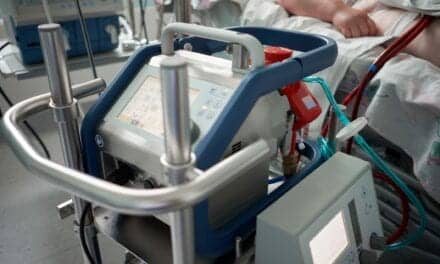
Doing the right thing for the patient is made easier by the best technology, and MeritCare has a commitment to the quality of its equipment as well as its staff. Currently, the facility’s RTs have access to a fleet of ventilators.
“MeritCare is very progressive,” Haberman says. “For instance, before inhaled nitric oxide was approved by the FDA [Food and Drug Administration], our staff members were sent to two centers where inhaled nitric oxide was being studied. With RTs’ technical support, pediatric cardiology moved forward obtaining a rescue protocol for inhaled nitric oxide use within our institution. Our NICU has used high frequency oscillatory ventilation [HFOV] technology since it has been FDA-approved, and RTs have been instrumental in our NICU’s participation in national studies to support the use of HFOV.”
Plans are under way to change the current fleet of ventilators in the very near future. The process of selecting new equipment involves an interdisciplinary team of 20 that includes therapists, physicians, nurses, managers, biomedical technicians, and members of the material services department.
“We have finished the first phase of our mechanical ventilator purchase, which involved an evaluation of what is on the market,” McCabe Halvorson says. “We are now in the second phase, evaluating new ventilators to use in critical care by doing a trial on some of the equipment on the market today. The core group processes all this information, and it’s interesting to get perspectives of different people on that team.”
Normally, Haberman and McCabe Halvorson work from a list of capital equipment items that the department needs annually. They meet with a maintenance therapist to get additional input, and can purchase equipment less than a certain dollar amount on their own.
“This is quite a significant purchase, however,” McCabe Halvorson says. “We are talking about replacing 18 or more ventilators in the near future. When trying to get our arms around how we are going to do this, especially when there are several good ventilators out there with similar characteristics, using the interdisciplinary team is a good process to follow.”
Special Programming
The department also stays at the forefront from an educational standpoint for its patients, particularly with its tobacco cessation program. North Dakota has a settlement fund through the public health department, and through its RT services involvement with public health, MeritCare was able to capitalize on some of the education offered. In place since the early 1980s, the tobacco cessation program is run out of the pulmonary laboratory and targets inpatients from the hospital’s heart services department.
“When we first started the program, we saw approximately 12 patients a month,” McCabe Halvorson says. “Now we see about 50 per month, most of whom are still inpatients in the heart services department.”
A referral is usually made to an RT, who determines a good time to meet with the patient and conduct a 1-hour counseling session. The program’s counseling is based on that performed at the Rochester, Minn-based Mayo Clinic, where MeritCare sends its RTs for training. The department then follows up extensively with its patients. A call is made 2 weeks after they are released from the hospital, then at 1 month, 3 months, 6 months, and 1 year later.
“We have had pretty good success with that program. In fact, our respiratory care services are really the resource for the entire health system when it comes to tobacco cessation,” McCabe Halvorson says. “There is a lot of information out there now about the health impacts of smoking. In the 1980s, it wasn’t so socially acceptable to discuss it, but now it’s a nice area for us to draw on. We have seen a lot of growth in that area over 15 years, and we anticipate that the program will eventually expand into other areas within the hospital’s inpatient population.
“It has become a natural function for us, and the amount of time involved is not extraordinary,” she adds. “We follow up using scripted phone calls, so an office member can do that task for 2 hours of her shift. The program has been pretty simple to implement, and I encourage other hospitals that have RTs with an interest in this realm to train them for it. Tobacco cessation is a real passion of mine and I enjoy working with this program.”
In It for the Long Haul
In fact, enjoying their work has been the one element that has kept McCabe Halvorson, Haberman, and Taylor at MeritCare for 23 years, 21 years, and nearly 20 years, respectively.
“What I like about MeritCare is the many opportunities,” McCabe Halvorson says. “We are able to try new procedures and techniques. We sometimes tend to think of MeritCare as being removed from it all, but that’s not the case. Here in Fargo, we are really doing quite a bit of the cutting edge in terms of respiratory care, from our TDPs to oscillators. We also have variability and flexibility for our therapists that are not always present in other RT departments.”
“MeritCare is a hospital in a city that is growing,” Haberman says. “We have new technology but we’re still on a first-name basis with our clients. These are small-town relationships where we work closely together and people treat one another with respect. That goes a long way.”
RT
Liz Finch is a contributing writer to RT Magazine. For more information, contact [email protected]