At Memorial Health University Medical Center, state-of-the-art technology—from new blood gas systems to network-wired information systems—stands side by side with a respiratory department that has increased levels in both efficiency and staff job satisfaction.
By Rich Smith
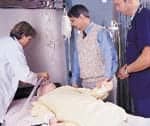
Stephen Morris, MD, and Linda Dominy stand beside a PACS station at Memorial Health University Medical Center in Savannah, Ga.
Waving good-bye to nearly a third of its therapists in a single day 2 years ago should have proved disastrous to the respiratory department at busy Memorial Health University Medical Center (MHUMC) in Savannah, Ga. It did not. At least not right away.
The therapists handed their walking papers were not let go; rather, they were reassigned and placed under the control of the pediatric hospital across campus. The reason: Respiratory care for children had grown so highly specialized that it was by then unrealistic to expect each therapist to be expert in treatment of both pediatric and adult patients, as had been department practice. It needed to be one or the other.
Administrators were confident they could operate an adults-only respiratory service with 30% fewer therapists, given that transferring the pediatric business to Backus Children’s Hospital at Memorial Health would mean a concomitant drop in total caseload. But a few months after those therapists departed, adult volume unexpectedly spiked. A year later the caseload for the 18-and-over demographic was back to where it had been prior to the staff divestiture, in effect leaving the department severely shorthanded—and without money to hire a sufficient number of replacements.
“We were in a real mess,” says Linda Dominy, RRT, MHA, manager of cardiopulmonary services within Memorial Health’s Heart and Vascular Institute, home of the respiratory department.
Solving that problem required several strategic moves on the part of respiratory. These included adoption of innovative technologies, wider use of advanced medications, and expansion of the list of therapist-driven protocols, all with the aim of increasing efficiency to help each therapist accomplish more in the same or less time than before.
When all was said and done, measurable efficiency had risen by 37% from the year before. This bore further fruit in the form of a $300,000 reduction in staffing costs, even after the therapists received pay raises. Meanwhile, an employee satisfaction survey taken in 2003, roughly 12 months following initial implementation of the efficiency initiatives, found staff happiness had risen from 3.72 to 4.38 on a scale of 1 to 5 (slight wonder, then, that Fortune Magazine chose Memorial Health as one of the nation’s top 100 places to work).
“Our therapists are working smarter, not harder,” says Dominy. “As a result, they’re enjoying their jobs more. And patients are benefiting from the improved quality of the product we offer.”
Empowered Therapists
MHUMC is a 530-bed, tertiary medical center with a level I trauma designation. It is the flagship facility of Memorial Health, a health delivery system serving a 35-county area of southeast Georgia and southern South Carolina, and stands as the area’s only teaching and research hospital (more than 300 clinical studies currently are open there).
The growth that threw the respiratory department’s operations for a loop was sparked when the hospital won a quick succession of managed care contracts.
“The first thing we did in response was increase the number of therapist-driven protocols we were using,” says Dominy. “The two most important were protocols covering vent weaning and asthma.”
John W. Bishop, CRRT, RRT, RCP, staff therapist assigned mainly to night duty in the adult ICU, explains that the new protocols help keep general-floor patients from remaining on therapy longer than necessary.
“They allow us to alert physicians at earlier junctures when the time has come to reduce the frequency or type of medications, or discontinue therapy entirely,” says Bishop. “Here in the ICU, we now have spontaneous breathing trials as part of our weaning protocol—tremendously valuable. In the past, we would have physicians ordering the patient weaned without providing us any specific goals or criteria. This protocol solved that problem.
“We also make extensive use of the ARDSNet protocol. People come in, they are difficult to oxygenate. We don’t want to keep them on high levels of PEEP and FIO2 so we simply order the ARDSNet protocol, provided they do not have any contraindicating hemodynamic problems. Patient FIO2 is weaned rapidly, PEEP is brought down, and they start to improve rapidly. These protocols have really made things more efficient for us.”
The department sought to boost efficiency as well by replacing traditional drugs with newer ones promising to work better or faster or both. One such changeover medication is levalbuterol (Xopenex).
“With a stabilized patient fresh out of critical care, levalbuterol dosing is only once every 6 to 8 hours instead of every 4,” says Dominy. “And we administer levalbuterol with a new, state-of-the-art nebulizer that delivers more medication to the patient in a shorter time—treatments normally taking 15 minutes can be administered in just 5.”
Thus, in a 24-hour cycle, a therapist now in many instances gives medications half as often and in sessions lasting a third as long, she indicates. The shorter treatment delivery spans make it practical for therapists to remain at the patient’s bedside the entire time; doing so even has become official departmental policy.
Therapists typically spend their bedside minutes conducting assessments, offering encouragement and education, or solving problems.
“A nice thing about the efficiencies all of this gives to us,” says Bishop, “is that we often have more time for exploring ways of doing things better for patients who don’t respond as well as we’d like to standard treatment.”
Online Anytime
MHUMC ranks among the nation’s 100 most extensively network-wired hospitals, according to Hospitals & Health Networks Magazine. Its massive information technology infrastructure supports an enterprise-wide patient electronic medical record (EMR) system accessible by respiratory therapists via terminals at the nurses’ stations on every floor and in the ICUs. Therapists use this EMR as a convenient, speedy means of documenting and of checking up on additions to their patients’ charts, such as newly reported laboratory values.
“Working with the information services department, we developed a customized EMR screen for our therapists,” says Dominy. “It’s arranged so that the items and tasks they most frequently access are the first things they encounter on the screen. This makes it a lot easier for them to get in and out of the chart. The system is set up so that as the therapists document, the charges are automatically compiled.”
(That auto-compilation feature has helped the department avoid failure to bill for services. In the year prior, lacking this capability, the department estimates that approximately $1 million worth of unbilled blood-gas charges alone slipped away.)
Also implemented was an upgraded computerized blood gas system. Before, therapists had to access up to three different computer systems to obtain the information they needed.
“The new system, by contrast, automatically runs the QCs for therapists every 4 hours during each shift,” says Dominy. “Blood gas numbers then automatically enter the EMR.”
A next step will be elimination of paper-based ventilator records.
“We’re working to have the ventilator parameters downloaded automatically into the computers so our respiratory therapists won’t have to write out any of that information while making rounds,” says Stephen L. Morris, MD, FACP, FCCP, medical director of respiratory care. “That is a capability we already have for ICU vital signs.”
Earlier, the hospital installed a radiology PACS (picture archiving and communications system) that allows digitally produced diagnostic images from x-ray, ultrasound, CT, MRI, and other modalities to be stored and distributed electronically. As with EMR data, respiratory therapists have access to those images.
“A therapist can pull up the patient’s chest image and, among other things, review it to observe lung condition or determine tube placement,” says Morris. “At present, images can not be accessed on handheld tablets; that is yet to come. For now, they can see images either at a PACS workstation—there is one on each floor—or on a PC connected to our intranet.
“No question about it, though. PACS has saved us a tremendous amount of time. We are no longer dealing with the problems of waiting for films to arrive, of searching for films that become misplaced or lost. We can look at images we need within seconds of requesting them.”
Another efficiency enhancer, PACS made possible respiratory’s development of a two-room bronchoscopy suite inside the endoscopy unit belonging to the MHUMC Cancer Institute.
“The dual rooms allow us to perform bronchoscopies on two patients concurrently—one patient without fluoroscopy, and a second with fluoroscopy by means of a dedicated C-arm,” Morris says. “Then, within the endoscopy suite, we have access to the PACS to look at radiographic imaging while we are doing the bronchoscopies, some of which involve use of argon-laser equipment for specialized studies. There’s also an area for prepping patients and for post-procedures.”
Previously, bronchoscopies were conducted in multiple locations, one of which was a room under the control of radiology. “We had to compete with the radiologists for time slots to do our procedures,” says Morris. “Now, with our bronchoscopy suite in a single location, we have full control over the timing of the procedures. That alone makes things a lot better for our patients.”
Going to the Top
Offered to therapists is participation in a clinical ladder program that supports their advancement professionally and financially. They climb the ladder—receiving commensurate increases in pay and a ceremonial award at each newly reached rung—by engaging in endeavors over and above those spelled out in their job descriptions. Examples would be the therapist who enrolls in classes to acquire added credentials, takes on special assignments that help the institution achieve its strategic goals, or suggests ways to help the enterprise save money, Morris outlines.
“It’s a mechanism that combines professional development with attempts at improving patient care,” he explains. “This, along with the general work environment we have created, contributes powerfully to the greater satisfaction the staff has these days.”
Bishop, the ICU-based therapist, agrees. “We are a trauma center, so we get patients who are the worst of the worst, but we are happier in our jobs because we feel that we have been both liberated and empowered by the efficiencies brought about by all the new technology and the other changes,” he says. “Because of the drive for greater efficiency, things have gotten so much better for us. And there is no sign of letup.” RT
Rich Smith is a contributing writer for RT.