Technology has brought great gains to the healthcare arena. Telehealth may take it to new heights.
By Carl Willoughby, RRT, RCP
We are living in an extraordinary time, a time of great changes. Some of those changes are political, some are social, some are technological, and all are interrelated. Electronic technology is advancing at a breathtaking pace and is bringing new and exciting possibilities to all areas of health care. Could we use technology, electronic communications, to provide pulmonary rehabilitation (PR) to patients?
Pulmonary rehabilitation is, for the most part, currently provided in an outpatient setting. Patients come to a program facility, usually hospital-based or hospital-supported, for a series of visits over several weeks. These visits provide the chronic respiratory disease patient with two things, both vital to improving their health. First, PR provides training for a much clearer understanding of their disease and how to handle it, ie, self-management. Second, PR provides individualized progressive exercise that puts the patient on a pathway to a lifetime home exercise plan.
 |
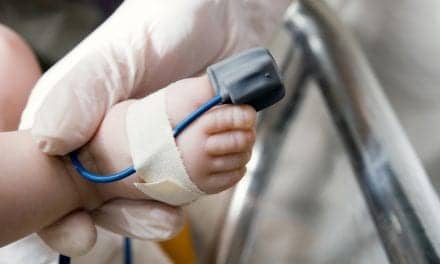
| Tina Jourdain demonstrates pulse oximetry to remote patients. |
The efficacy and value of PR are no longer in dispute. The last 2 decades have seen an accumulation of scientific literature that clearly demonstrates the benefits. The American Thoracic Society/European Respiratory Society Statement on Pulmonary Rehabilitation says it well1: “Evidence-based support for pulmonary rehabilitation in the management of patients with chronic respiratory disease has grown tremendously, and this comprehensive intervention has been clearly demonstrated to reduce dyspnea, increase exercise performance, and improve health-related quality of life (HRQL). Furthermore, an emerging literature is beginning to reveal its effectiveness in reducing health care costs.”
We have an effective tool to help chronic respiratory disease patients, and yet very few of those patients have access to PR. In a recently published Canadian study,2 François Maltais, MD, estimates that only 1% to 2% of the Canadian COPD population has access to PR. The numbers for the United States may be slightly higher, but they almost certainly are in the low single digits as a percentage.
How can we reach out to those rural patients who do not have access to PR simply because there are no programs nearby?3 This became a very real question for me a few weeks ago when a distant university hospital called us with a COPD patient referral.
Now, I am used to having patients referred to our small, but busy, pulmonary rehabilitation program at Mad River Community Hospital in rural Northern California. However, this referral was different. The patient lives more than 80 miles to the north and has limited access to transportation. I was being asked if we could provide all or part of his pulmonary rehabilitation via telemedicine.
This was definitely a new area for us and, as I soon found out, for most of the pulmonary rehabilitation community. The obvious first step was to gather information—do my homework. That is when I began to learn about the exciting possibilities of telemedicine.
As with many areas of health care, the terminology can be confusing, and often telemedicine and telehealth are used interchangeably.
The American Telemedicine Association provides the following definitions4: “Telemedicine is the use of medical information exchanged from one site to another via electronic communications to improve patients’ health status. Closely associated with telemedicine is the term ‘telehealth,’ which is often used to encompass a broader definition of remote healthcare that does not always involve clinical services. Videoconferencing, transmission of still images, e-health including patient portals, remote monitoring of vital signs, continuing medical education, and nursing call centers are all considered part of telemedicine and telehealth.”
The use of telemedicine reaches much further back than you might imagine. The California Telemedicine & eHealth Center5 provides us with some interesting history, “There had been experiments using radio telecardiology (from the 1910s), telephone-mediated telestethoscopy (from the 1920s)…. The first generation of telemedicine using video conferencing began in the late 1950s.”
Since the mid 90s, the use of telemedicine programs has grown dramatically, representing nearly every area of health care and a wide variety of specialties. Telemedicine is being employed by radiology, pathology, continuing education, cardiac monitoring, psychiatric care, home care, emergency care, and various surgical specialties, including robotic surgery.
Telemedicine is represented by established professional societies6 and other organizations such as the American Telemedicine Association, the Association of Telehealth Service Providers, and the Telemedicine Information Exchange. There are publications of standing, such as the European Journal of Telemedicine and Telecare.
The American Association of Cardiovascular and Pulmonary Rehabilitation published a “Telemedicine Position Statement” in 2001.7 It reads in part: “The American Association of Cardiovascular and Pulmonary Rehabilitation (AACVPR) recognizes the value of advancing technology and the benefits it may provide in the delivery of cardiac and pulmonary rehabilitation services.”
What Would Pulmonary Rehabilitation via Telemedicine Look Like?
Pulmonary rehabilitation is one service very much underrepresented in the rapidly growing world of telemedicine. Although many PR programs use video resources and telephone follow-ups, and refer patients to Internet resources, I was able to find only one program with a fully dedicated and organized approach to delivering pulmonary rehabilitation by telemedicine, the Caritas Centre for Lung Health’s “Breath Easy” TelePulmonary Rehabilitation Program based in Edmonton, Alberta.
In a telephone interview, Tina Jourdain, RRT, the coordinator of the Caritas TelePulmonary Rehabilitation Program, was kind enough to share the story of how she is using telemedicine to serve COPD patients scattered across Alberta. The Caritas Centre PR program has been serving the Edmonton area for more than 15 years. In 2005, with grant support from Alberta Health and Wellness, Fred MacDonald, MD, established the TelePulmonary Rehabilitation Program.
The program structure is similar to other outpatient programs. Patients come to a health care clinic or facility, near their home, where the telemedicine equipment is located. A two-way, high-speed, high-definition, encrypted link provides both video and audio between the PR provider in Edmonton and the patients who may be hundreds of miles away. The live interactive connection allows for education and training just as with a face-to-face on-site visit.
Jourdain’s patients are scheduled for telehealth visits twice a week for 8 weeks. Most visits consist of 1 hour for education/training and 2 hours for moderate-paced exercise. The exercise is conducted at the local facility, where the patient is located, and monitored by a local RRT, physical therapist, or registered nurse who has been approved by Caritas TelePulmonary Rehabilitation. At the end of 8 weeks, the patients have established exercise plans they can carry out in their community or at home. There is also a schedule of postprogram follow-up contacts by telephone.
The Caritas TelePulmonary Rehabilitation Program is gaining acceptance from both patients and physicians. “Country patients have done very, very well,” says MacDonald. “We have the patients now telling us what a joy it is that they don’t have to go into Edmonton and can exercise in their own community.”
So What’s Holding Us Back? Are There Any Problems? Obstacles?
What about patient safety and legal risks? Can you recommend exercise to a patient when you are physically far away when there might be is a problem? The Caritas TelePulmonary Rehabilitation Program solved this by having a trained licensed provider present at the remote location. Just as with our traditional outpatient PR, at the end of the program the patient is discharged with a safe and practical home exercise plan.
Here in the United States, one of the first issues raised is reimbursement. Most PR patients are covered under Medicare. Will CMS (Medicare) reimburse for PR provided by telemedicine to a patient at an off-site location? Currently, CMS reimburses for a whole variety of procedures such as physician office visits, specialty consultations, radiology, and mental health and nutritional evaluations. In most cases, the reimbursement is just as if the provider and patient were not separated by distance.
CMS is in the midst of transitioning from the old Fiscal Intermediary system to the new Medicare Administrative Contractor system. Some of the MACs are just now figuring out how to deal with conventional PR claims.8
The question remains. Since it has not been done before, how will CMS, in the person of a MAC claims reviewer, view a claim for providing PR by telemedicine? Hopefully, CMS will reimburse just as for an on-site visit, but we probably will not know until it is tried.
When it comes to the necessary broadband networks, the Federal Communications Commission (FCC) has been an active proponent of establishing state and regional networks. The Telecommunications Act of 19969 resulted in funding up to $400 million, and pilot programs are now under way in many states. In a 2007 press release,10 FCC Chairman Kevin J. Martin said, “With this pilot program, the Commission will be taking a major step toward the goal of connecting health care facilities across the nation with one another through broadband telehealth networks for the benefit of patients.”
Now it is up to us, the PR providers. It is time to advance the concept of using telemedicine to reach those respiratory patients who will otherwise go untreated. We need to open up dialogue on this topic with each other, with our physician medical directors, with hospital administrators, and with those responsible for reimbursement.
By the time you read this article, I hope to have the PR telemedicine program at Mad River Community Hospital in place and have completed working with my first telemedicine pulmonary rehabilitation patient.
RT
Carl Willoughby, RRT, RCP, is pulmonary rehabilitation coordinator, Mad River Community Hospital, Arcata, Calif. For further information, contact [email protected].
References
- Nici L, Donner C, Wouters E, et al. American Thoracic Society /European Respiratory Society Statement on Pulmonary Rehabilitation. Am J Respir Crit Care Med. 2006;173:1390-1413.
- Maltais F, Bourbeau J, Shapiro S, et al. Effects of home-based pulmonary rehabilitation in patients with chronic obstructive pulmonary disease. Ann Intern Med. 2008;12:869-78.
- Challenges facing rural hospitals. AHA Trend Watch, American Hospital Association. 2002;4:1-8.
- American Telemedicine Association. Available at: www.americantelemed.org. Accessed December 13, 2008.
- California Telemedicine & eHealth Center. The History of Telemedicine. Available at: www.cteconline.org. Accessed December 17, 2008.
- Telemedicine Information Exchange. Available at: wwwltie.telemedicine.org. Accessed December 9, 2009.
- Shaw KD, Heggestad-Hereford JR, Southard DR, Sparks KE. American Association of Cardiovascular and Pulmonary Rehabilitation Telemedicine Position Statement. J Cardiopulm Rehabil. 2001;21(5):261-2.
- Centers for Medicare and Medicaid Services. Request for adding services to the list of Medicare telehealth services. Available at: www.cms.hhs.gov/Telehealth/04_Criteria.asp. Accessed December 8, 2008.
- Federal Communications Commission Rural Health Care Support Mechanism for Telehealth. Available at: www.ncsl.org/statefed/health/FCCRuralHlth.htm. Accessed December 8, 2008.
- FCC News. FCC Chairman Martin Discusses Benefits of Deploying Broadband Telehealth Networks in Rural and Underserved Communities. November 13, 2007. Available at: www.fcc.gov. Accessed December 17, 2008.